Choosing Family Medicine First:
A reflection on trends for graduates of Canadian and international medical schools
By Steve Slade | April, 2026
As data and information consumers we learn quickly that diverging and converging trend lines generally mean something. They pique interest and make us wonder what’s going on behind the data, what’s driving the trend. They may confirm or challenge our impressions. They can raise concerns or signal progress being made. They flag something that needs talking about.
The following trend lines do that for me, and maybe you too.
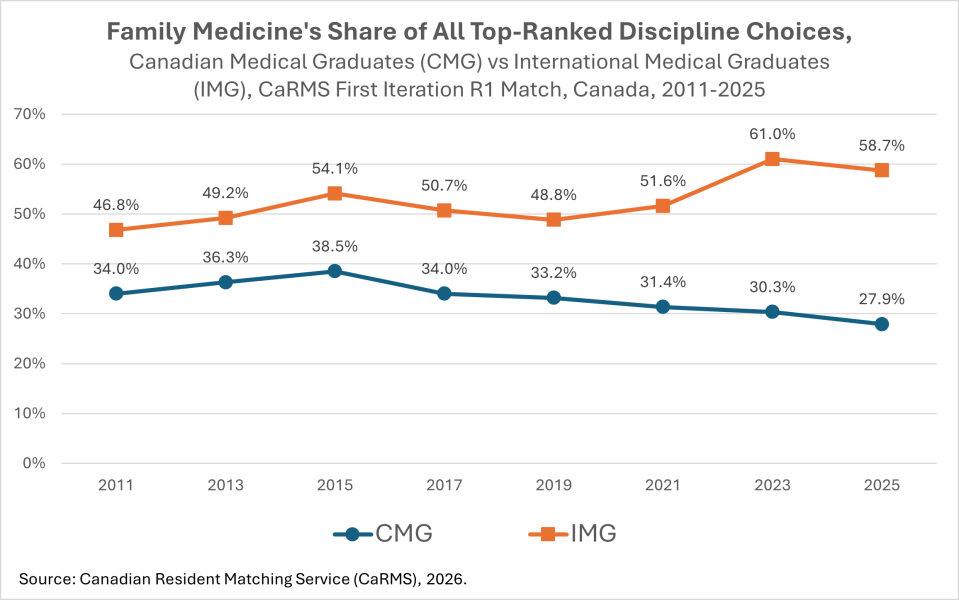
This data is from the Canadian Residency Matching Service (CaRMS), which is the gateway to specialized residency training in Canada. As part of the CaRMS process, medical graduates select one or more disciplines and training programs, indicating their topmost and lesser preferences as they do so. The figure shows that, among graduates of international medical schools (IMGs), family medicine accounts for an increasing share of the disciplines ranked first. Among graduates of Canadian medical schools (CMGs), family medicine accounts for a decreasing share of top-ranked choices.
These trend lines cut through an era of increasing primary care crisis in Canada, a crisis that is defined by both population healthcare needs and health workforce challenges. We are in a time where we increasingly look to IMGs for relief. Against this backdrop, the diverging trajectories demand consideration of what is driving the trends and what, if anything, might be done to adjust their course.
1. The IMG trend is, in many ways, congruent with what we are observing across the system. Canada is leaning more heavily on IMGs, and family medicine is front-and-centre in workforce planning conversations. IMGs may be responding to that reality—seeing clearer pathways into practice or more targeted recruitment and bridging supports in primary care. If family medicine is increasingly positioned as the place where IMGs are most needed, it is not surprising to see that reflected in their first-choice rankings.
2. The CMG pattern is more perplexing. Despite our intense concern about access to primary care, relatively fewer CMGs are ranking family medicine as their top choice. One plausible explanation is that CMGs are more tuned in to the prevailing narrative about family practice in Canada—often a narrative dominated by heavy workloads, administrative burden, burnout, and poor pay. Those issues are real. But when they become the whole story, they distort perceptions and, understandably, how medical students would weigh their discipline choices.
As a long-time data user I know that, across broad sources, the data has a much better story to tell about family medicine. Data published by the Association of Faculties of Medicine of Canada show that medical students have their best experiences in family medicine. Data from The College of Family Physicians of Canada shows that almost all family medicine residents are proud to become family doctors. The Canadian Medical Association’s National Physician Health Survey shows high levels of wellness among family physicians—higher than other physicians and surgeons. At a systems level, many jurisdictions are taking concrete steps to strengthen primary care through payment reform. Also, family physicians have broad professional latitude: while they are core primary care providers, many also practice in emergency rooms, hospital inpatient wards, care homes, and other settings. In other words, family practice is demanding, but it is also diverse, portable, intrinsically rewarding, and of great value to patients and the healthcare system.

Telling this better story of family medicine matters for many reasons. If IMGs are increasingly selecting family medicine first while CMGs are doing so less often, we may be drifting toward a two-track model of workforce supply—one in which primary care depends disproportionately on IMGs. That may be a necessary reality in the short term, but it raises longer-term questions about sustainability, equity, and retention. At the same time, the unduly negative story of family practice may dissuade CMGs from a career path that would bring great professional satisfaction.
The CMG-IMG trend lines push us to think about who sees family medicine as their best first choice—and why. In many ways the IMG trend adds up, but the CMG trend is puzzling and suggests the need for a more accurate, data-driven narrative about family practice—one that reflects not only pressures, but also wellness, reform, and professional latitude. A more balanced, evidence-informed narrative about family practice would point to progress that is being made. It could buoy those who work in family medicine today. Perhaps most importantly, it would better serve medical students in Canada as they consider their career choices. It would give reassurance that it’s not wrong to feel good about choosing family medicine first.
Perspectives from CHWN Leads
Maria Mathews | Primary Care Co-Lead
Maybe it’s time that we revisit our assumptions about what these statistics imply for CMGs. Often, we assume that a large number of students entering medical school want to become family physicians… and that we lose them to other specialties over the course of medical school. Maybe we should instead think about our success in retaining the number of students who enter medical school with an interest in family medicine.
To understand whether we are gaining or losing students interested in family medicine, we need to measure interest in family medicine when students first start medical school. A survey of first-year students’ interests at the start of medical school would allow us to better understand whether 27.9% means we’ve lost, retained, or gained students interested in family medicine over the course of their medical school training. Such a survey would also help us understand whether initiatives to expose students to family medicine — such as longitudinal placements, generalist-oriented schools, family medicine interest groups, and family medicine-specific training sites, to name a few — make a difference. Now if only we knew someone with the influence and connections to introduce a first-year medical student survey… any ideas, Steve Slade?"
Lindsay Hedden | Primary Care Co-Lead
Dr. Mathews raises an important methodological point: without a baseline measure of interest at entry to medical school, we can't know what's driving the CMG trend, or where along the training trajectory to intervene. But the data also push us to ask a harder structural question: even if we could shift narratives and rekindle interest in family medicine among CMGs, are we offering a practice model that would retain it? Research consistently shows that physicians, particularly those newer to practice, want to work in interdisciplinary teams, with reduced administrative burden, and in employment-based models rather than as small business owners. Until the structure of family practice better reflects what CMGs are actually looking for in a career, a better story alone may not be enough.
Houssem Eddine Ben-Ahmed | Mobility, Migration & Integration Lead
I appreciate Steve’s reflection on the topic of family medicine and the important observations raised by Dr. Mathews and Dr. Hedden. As Lead of the Mobility, Migration and Integration Policy Theme at CHWN, I strongly believe that this reflection comes at the right time, as Canada is facing a critical and growing shortage of primary healthcare workers. In recent years, Canada has depended heavily on IMGs, who are making critical contributions to strengthening access to care and supporting the health system. At the same time, this trend raises important ethical concerns. While reliance on IMGs may offer short-term relief for Canada, it can also have negative consequences for source countries—many of which are already experiencing significant workforce shortages. This suggests the importance of reviewing workforce planning approaches through an equity lens. I find Steve’s reflection very interesting, as it invites us to think about how we can strengthen family medicine as an appealing choice for Canadian medical graduates and challenge negative perceptions of the field to make it a more attractive career choice for future physicians.
Steve Slade, Director of Research, The College of Family Physicians of Canada (comments and opinions are my own and may not reflect those of my employer or the Canadian Health Workforce Network)
